Translate this page into:
Proton Pump Inhibitors: Uncovering the Mystery Behind Refractory Severe Hypocalcemia - A Case Report
Corresponding author: Sagar Sangole Seth G. S. Medical College and KEM Hospital, Mumbai, India Email ID - docsagarmd@gmail.com
-
Received: ,
Accepted: ,
Abstract
Proton pump inhibitors (PPIs) are commonly prescribed drugs to reduce gastric acid secretion and treat a variety of gastrointestinal disorders. Hypomagnesemia has been reported with long-term PPI use. We report a case of long-term PPI use associated with refractory severe hypocalcemia secondary to a normo-magnesemic tissue magnesium deficiency. The patient presented with clinical symptoms of spasms and perioral tingling along with prolongation of QTc interval on electrocardiogram. On failure of intravenous (IV) calcium therapy, the patient improved after a trial of IV magnesium therapy. It is crucial in clinical practice to be aware of adverse events of long-term PPI therapy.
Keywords
Carpopedal spasm
Chvostek sign
Magnesium Sulfate
Pantoprazole
Proton Pump Inhibitor
Tetany
Trousseau sign
INTRODUCTION
Proton Pump Inhibitors (PPI) are commonly prescribed drugs that act by inhibiting H(+)-K(+)-Exchanging ATPase. These drugs, which are prescribed for gastroesophageal reflux disease, peptic ulcer disease, etc., are associated with various adverse effects. Hypomagnesemia has been reported with long-term PPI use.1 However, the incidence rate and mechanism are still unclear.2 Hypomagnesemia, may cause neuromuscular and cardiac complications, hypoparathyroidism, bone metabolic diseases, and concurrent electrolyte disorders (mainly hypocalcemia and hypokalemia).3 Here, we report a case of long-term PPI use associated with refractory severe hypocalcemia that improved after a trial of intravenous (IV) magnesium in a patient with a normo-magnesemic tissue magnesium deficiency.
CASE REPORT
A 65 year old female, presented to the emergency department with perioral tingling sensations for 5 days and spasms in her hands for 2 days. She has had a history of gastroesophageal reflux disease (GERD) and dyspepsia for 10 years, for which she has been taking Tab. Pantoprazole 40 mg PO OD. She was not suffering from any other comorbid conditions. Also no history of diuretic or recent antimicrobial agent use and no history suggestive of malabsorption syndromes. She also denied any history of alcohol, tobacco and recreational drug abuse. On examination, the Chvostek sign and Trousseau sign (Figure 1) were positive. No other significant findings were observed on examination. Laboratory investigations are mentioned in table 1.
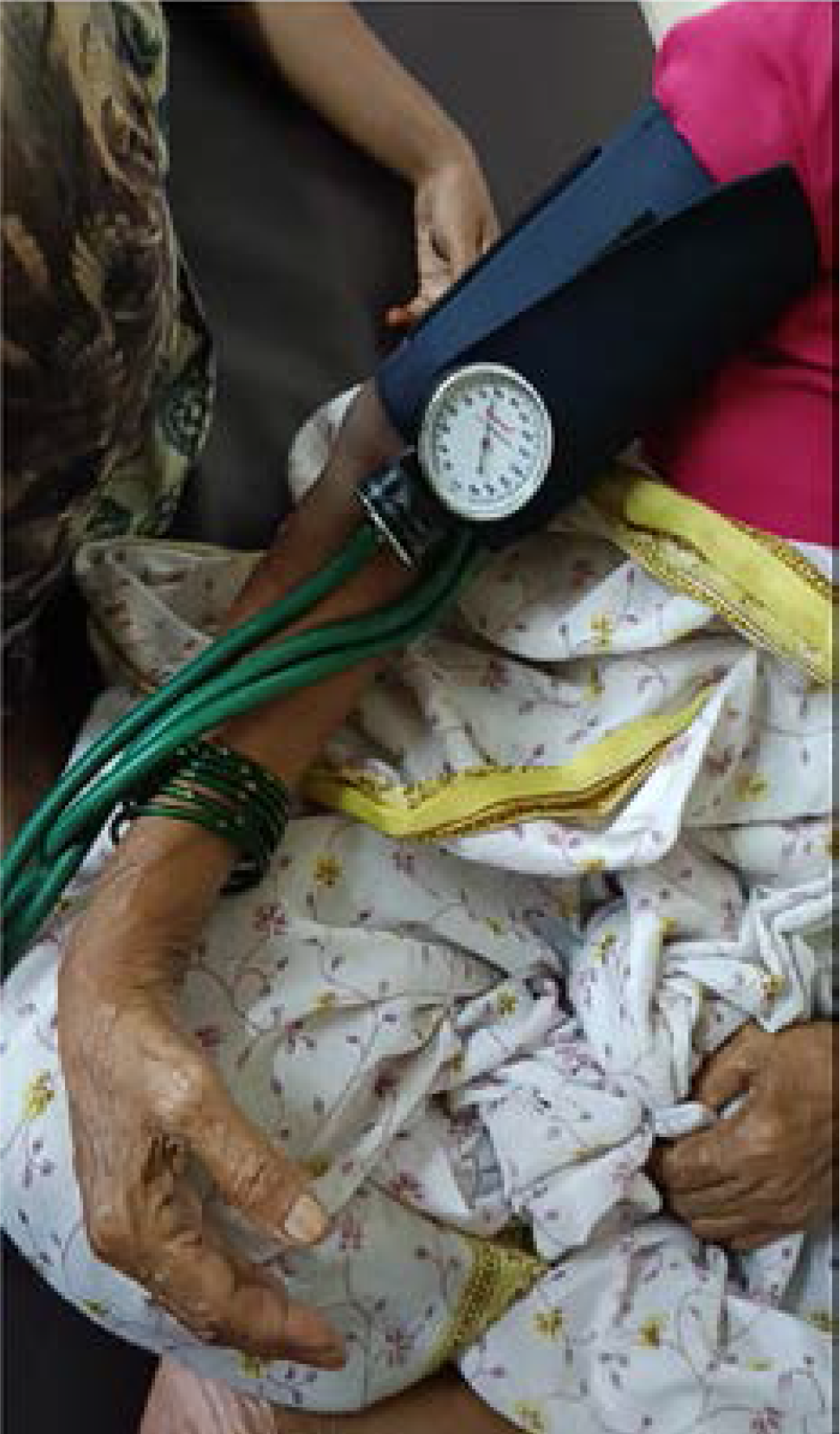
- Showing a positive Trousseau’s sign for latent tetany in the setting of hypocalcemia. The sign is observable as a carpopedal spasm induced by ischemia secondary to the inflation of a sphygmomanometer cuff to 20 mmHg over the systolic blood pressure for 3 minutes
| Laboratory Parameter | Result | Laboratory Refer-ence Range |
|---|---|---|
| 25-OH Vit D | 22 ng/ml | 22- 40 ng/ml |
| Albumin | 3.5 g/dl | 3.5 to 5.0 g/dl |
| Calcium | 6.6 mg/dl* | 8.5–10.5 mg/dL |
| Chloride | 101 mEq/L | 96 to 106 mEq/L |
| Free T3 | 2.600 pg/ml | 2.3-6.6 pg/ml |
| Free T4 | 1.100 ng/dl | 0.8-1.8 ng/dl |
| Ionised Calcium | 0.54 mmol/lit* | 1.12-1.32 mmol/lit |
| Magnesium | 1.8 mg/ml | 1.6-2.8 mg/dl |
| Phosphorus | 3.3 mg/dl | 2.5–4.5 mg/dL |
| Potassium | 3.6 mEq/L | 3.5-5.2 mEq/L |
| Serum PTH | 10.3 pg/dl* | 11-69 pgm/dl |
| Sodium | 137 mEq/L | 135-145 mEq/L |
| Total Proteins | 6.3 g/dl | 6 to 8 g/dl |
| TSH | 7.170 uIU/ml | 0.4-4 uIU/ml |
| Urinary Calcium | 2.16 mg/dl* | 4.5 – 5.3 mg /dl |
| Male Literacy Rate (%) * | 88.33 | 82.14 |
| Female Literacy Rate (%) * | 70.70 | 65.46 |
The electrocardiogram (ECG) had QT prolongation (Figure 2). Arterial blood gas analysis and kidney and liver function tests were normal. The laboratory investigations are as shown in Table 1. Renal ultrasound was normal. Various tests to rule out etiology of hypocalcemia were normal or borderline normal as seen in Table 1.
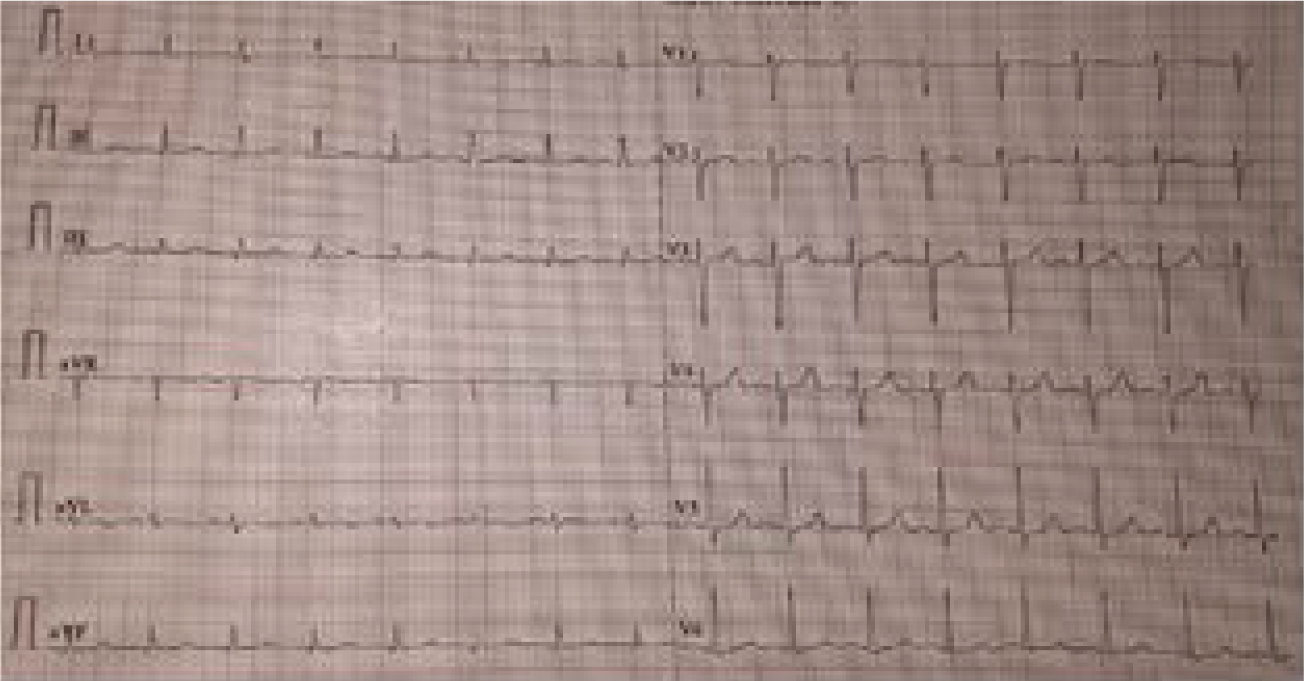
- Electrocardiogram (ECG) at the time of presentation showing prolonged QTc interval (480 msec)
The patient was treated with IV calcium gluconate (90 mg elemental calcium given over 20 minutes, followed by a repeat dose after 60 minutes, followed by 2400 mg elemental calcium over 48 hours at a rate of 50 mg/hr). Over the next two days, there was no significant improvement in both clinical symptoms and the serum calcium level. Considering the possibility of tissue magnesium deficiency, she underwent a trial of IV magnesium sulphate (2 g/day for 2 days). After 24 hours, the ECG changes reverted (Figure 3), and she became asymptomatic. This therapeutic trial affirmed us to possibly ascertain the cause of hypocalcemia to be tissue magnesium deficiency. She was continued on oral calcium and magnesium supplements and was observed for the next two days. She remained asymptomatic and was later discharged. She was advised to stop PPI, make lifestyle modifications with respect to GERD, and take antihistamine drugs (Ranitidine) as needed. On a follow-up visit after 3 months, she had normal serum calcium levels.
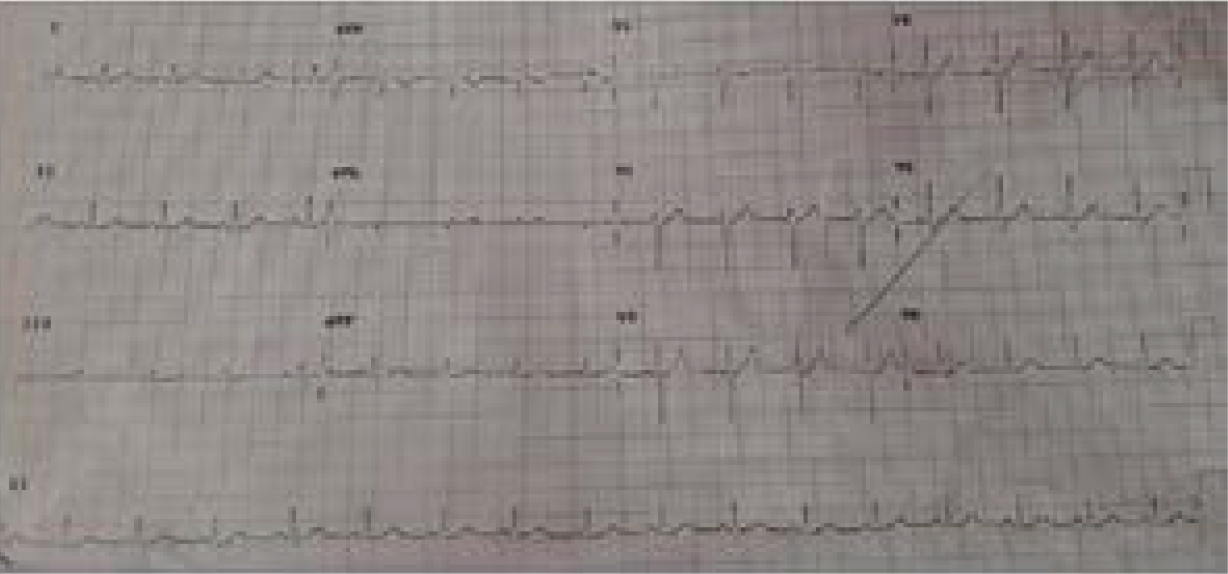
- Electrocardiogram (ECG) 24 hours after IV Magnesium therapy showing normal QTc interval (<460 msec)
DISCUSSION
Proton pump inhibitors (PPIs), with or without prokinetic agents, are now among the most rampantly prescribed drugs.4 They are used to reduce gastric acid secretion and treat a variety of gastrointestinal disorders, such as GERD, peptic ulcer disease, and Helicobacter pylori infection. However, a recent meta-analysis has shown that PPI use is associated with an increased risk of hypomagnesemia, a potentially serious electrolyte imbalance.5 In current clinical practice, many patients with symptomatic GERD are treated empirically with medications without prior endoscopy, i.e., without knowledge of whether the patient has erosive or nonerosive reflux disease.6
Severe hypocalcemia, which is defined as serum calcium <7.6 mg/dL, is an emergency with the risk of life-threatening cardiac arrhythmias or seizures. Refractory hypocalcemia is resistant to standard intravenous calcium therapy. The possibility of normo-magnesemic magnesium depletion (in which there is isolated cellular magnesium depletion) should be considered as a possible cause of refractory hypokalemia or unexplained hypocalcemia in patients at high risk for magnesium loss.7 The concentration of serum magnesium is closely regulated. Because only 1% of body magnesium resides in the extracellular fluid, measurements of serum magnesium levels may not accurately reflect the level of total body magnesium stores. Hypomagnesemia is defined as a serum magnesium level below the normal range of 1.7 to 2.2 mg/dL. The symptoms of hypomagnesemia can range from mild muscle weakness and cramping to seizures, cardiac arrhythmias, and even death. Several case reports and observational studies have linked PPI use to hypomagnesemia, with some studies reporting an incidence as high as 50% in patients on long-term PPI therapy.8
The mechanism by which PPIs cause hypomagnesemia is not fully understood, but several hypotheses have been proposed.9 One theory suggests that PPIs may interfere with the absorption of magnesium in the gastrointestinal tract by reducing the acidity of the stomach, which is necessary for the solubilization and ionization of magnesium salts. Another theory suggests that PPIs may affect the expression of certain transport proteins involved in magnesium homeostasis, leading to decreased magnesium reabsorption in the kidneys.10
Despite the growing body of evidence linking PPI use to hypomagnesemia, the true incidence of this adverse effect is still unclear, and more research is needed to fully understand the underlying mechanisms. However, it is important for clinicians to be aware of this potential risk and to monitor patients on long-term PPI therapy for signs and symptoms of hypomagnesemia.
CONCLUSION
In conclusion, PPIs are a widely prescribed class of drugs that have been shown to be effective in treating a variety of gastrointestinal disorders. However, their use has been associated with an increased risk of hypomagnesemia, which can have serious consequences if left untreated. Clinicians should be aware of this potential adverse effect and monitor patients on long-term PPI therapy for signs and symptoms of hypomagnesemia. The possibility of normo-magnesemic magnesium depletion should be considered as a possible cause of refractory hypokalemia or unexplained hypocalcemia in patients at high risk for magnesium loss.
END NOTE
Author Information
Sagar Sangole, Seth G. S. Medical College and KEM Hospital, Mumbai, India Sushrut Ingawale, Quinnipiac University Frank H. Netter, MD, School of Medicine / St. Vincent Medical Center, Connecticut, USA Kaustubh Salagre, Seth G. S. Medical College and KEM Hospital, Mumbai, India Mrunal Narkhede, Seth G. S. Medical College and KEM Hospital, Mumbai, India
Conflict of interest
None declared
References
- Magnesium Deficiency and Proton-Pump Inhibitor Use: A Clinical Review. J Clin Pharmacol. 2016;56(6):660-8. Epub 2015 Dec 30
- [CrossRef] [PubMed] [Google Scholar]
- Hypomagnesemia and proton-pump inhibitors. Expert Opin Drug Saf. 2013;12(5):709-16. Epub 2013 Jun 29
- [CrossRef] [PubMed] [Google Scholar]
- Treatment of hypomagnesemia. Am J Kidney Dis. 2014;63(4):691-5. Epub 2013 Oct 4
- [CrossRef] [PubMed] [Google Scholar]
- Prescription pattern & adverse drug reactions of prokinetics. Indian J Med Res. 2019;149(6):748-754.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Proton pump inhibitors and hypomagnesemia: A meta-analysis of observational studies. Medicine (Baltimore). 2019;98(44):e17788.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Gastro-oesophageal reflux disease. Nat Rev Dis Primers. 2021;7(1):55.
- [CrossRef] [PubMed] [Google Scholar]
- Hypomagnesemia: a clinical perspective. Int J Nephrol Renovasc Dis. 2014;7:219-30.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Proton pump inhibitors and severe hypomagnesaemia. Curr Opin Gastroenterol. 2016;32(2):105-9.
- [Google Scholar]
- Proton-pump inhibitors and hypomagnesemic hypoparathyroidism. N Engl J Med. 2006;355(17):1834-6.
- [CrossRef] [PubMed] [Google Scholar]
- A case series of proton pump inhibitor-induced hypomagnesemia. Am J Kidney Dis. 2010;56(1):112-6.
- [CrossRef] [PubMed] [Google Scholar]






